Small dense LDL, sub-clinical atherosclerosis and psoriatic arthritis
Psoriatic arthritis (PsA) is a chronic arthropathy associated with psoriasis, marked by an axial and/or peripheral joint involvement and high cardiovascular.
Several large studies confirmed the relationship of small dense LDL (sd-LDL) with coronary events. Although some studies examined the lipid profile in PsA patients, no data are currently available on a possible relationship of high levels of sd-LDL with PsA. The aim of the present study was to evaluate the concentration of sd-LDL in PsA patients and to assess the relationship with carotid intima-media thickness.
After excluding those already under treatment with statins and those with a known diagnosis of alterations in lipid metabolism (n=33), 50 PsA subjects and 100 matched controls were enrolled in this study. Among the 50 PsA patients, 23 were receiving Disease-Modifying Antirheumatic drugs (DMARDs) and 27 were under TNF-α blockers. None of PsA patients were receiving combined treatment with DMARDs+ TNF-α blockers. Minimal disease activity was found in 16 PsA patients (7 under DMARDs and 9 under TNF-α blockers).
Major clinical, biochemical and demographic characteristics of the two study populations are reported in Table 1. Triglycerides, Apo B, BMI, HOMA, and the prevalence of MS and Carotid plaques were significantly lower in the control group as compared to PsA patients; 21 (42.00%) out of 50 PsA patients had axial and 28 (58.00%) had peripheral subset; among these 15 (30.00%) had oligoarticular and 14 (28.00%) polyarticular involvement.
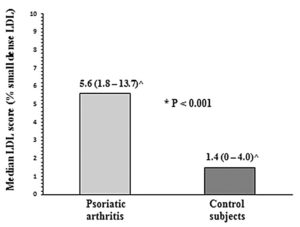
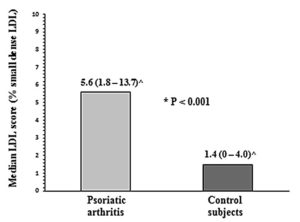
Median LDL score was significantly higher in patient with PsA as compared to control group (median 5.6 vs. 1.4, p<0.001) (Fig. 1).
All results were confirmed when stratifying analyses according to the type of treatment [(DMARDs) vs TNF-α blockers] or according to disease activity [minimal disease activity (MDA) vs active disease (AD)].
In Multivariate logistic analysis , after controlling for age and gender LDL score (below or above the 75th percentiles of the control values) is independently related to PsA diagnosis (OR 3.94; 95% CI 1.86–8.32; p<0.001 for PsA diagnosis). This relation was confirmed after controlling for age, gender, PsA diagnosis and MS diagnosis (OR 3.22; 95% CI 1.47–7.03; p=0.003 for PsA diagnosis).
The carotid ultrasound examination showed that carotid plaques were reported by 38% of PsA patients and 14% of controls (OR: 3.93, 95%CI: 1.61-9.60, p = 0.003) . Moreover, LDL score and LDL diameter significantly and directly correlated with the carotid Intima Media Thickness in patients with PsA.
The present study shows a novel relationship between sd-LDL and PsA diagnosis and sub-clinical atherosclerosis. This relationship is independent of the presence of Metabolic Syndrome; almost 26 % of studied PsA patients were diagnosed as having MS;
Our study indicates that patients with PsA have an increased concentration of sd-LDL independently of the presence of Metabolic Syndrome, this data suggests a possible link between PsA and the development of atherosclerosis mediated by sd-LDL. LDL size measurement gives potentially useful information in the risk assessment for atherosclerotic disease in these patients and could be useful in identifying a subsample of high risk patients, with prominent lipoprotein abnormality, among those with the PsA diagnosis, deserving lipid-lowering intervention. This hypothesis has, however, to be further tested with prospective epidemiological studies.
Marco Gentile
Department of Clinical Medicine and Surgery, University Federico II, Naples, Italy
Publication
Association between small dense LDL and sub-clinical atherosclerosis in patients with psoriatic arthritis.
Gentile M, Peluso R, Di Minno MN, Costa L, Caso F, de Simone B, Iannuzzo G, Scarpa R, Rubba P
Clin Rheumatol. 2016 Aug




![Can [60]fullerene maintain good health and prolong lifespan? AoS. Can [60]fullerene maintain good health and prolong lifespan?](https://atlasofscience.org/wp-content/uploads/2022/03/Can-60-fullerene-maintain-good-health-AoS-t-65x65.jpg)








Leave a Reply
You must be logged in to post a comment.