Adverse Drug Reactions: power, harm reduction, regulation and the ADRe profile
Patients should be checked systematically to ensure that they are not being harmed by their medication. Through case studies of prescriptions of antipsychotics to older adults in the UK, we have shown that if healthcare professionals systematically checked, harm could be prevented.
Healthcare professionals often place too much faith in the medication they prescribe. Prescribed medicines benefit between 4% and 25% of patients, but the harm caused by adverse drug reactions (ADRs) can outweigh these benefits. For example, 11% of hospitalised patients experience adverse effects from their medication, with 0.25% dying of ADRs. Up to 37% of patients with cognitive impairment may experience similar kinds of harm. Yet healthcare systems have failed to adopt standard procedures for checking for these harms, with many professionals finding it difficult to distinguish the negative effects of medication from other forms of illness. This, in turn, gives rise to more prescriptions, and more harm from medication.
ADRs are a drain on healthcare resources, causing 5-8% of unplanned hospital admissions, rising to 10% in older adults. This costs the UK’s National Health Service up to £1.6bn each year. Even this statistic may not represent the full problem: up to 60% of cases where patients are harmed by their medicines go unrecognised and unreported. The introduction of a comprehensive and systematic approach that bridges across healthcare professions would go a long way towards addressing these preventable problems.
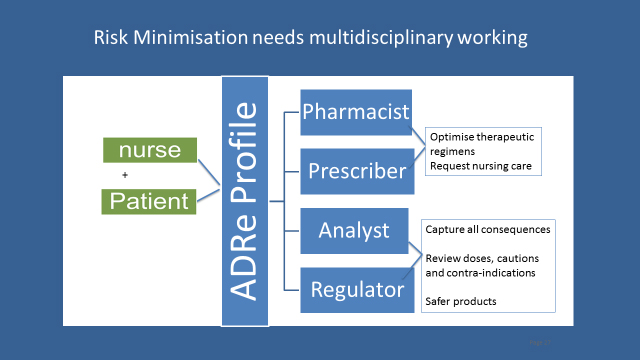
Our solution is the Adverse Drug Reaction (ADRe) Profile. It asks nurses to systematically check patients for an itemised set of adverse or undesirable effects of their mental health medicines. It also asks them to take action in case of problems, and, crucially, to share that information with pharmacists or those prescribing medicines. It formalises and standardises the approach to monitoring patients prescribed mental health medicines (Fig. 1).
The profile asks nurses to check vital signs, and all the signs and symptoms associated with potential adverse side effects. Nurses then document observations, plus any changes ADRs (Fig. 2). ADRe also covers key areas of wellbeing affected by medicines, including diet, non-prescription medicines, service user’s perspectives, and modifications to an individual’s care plan. Nurses then pass this completed profile to pharmacists and prescribers, to inform reviews of individual patients’ medication. The profile enables a deeper analysis of patients’ problems, and enables medication to be changed to avoid harm to patients.
We found clear benefits to this approach in our case studies and randomised controlled trials. The ADRe Profile collects data on patient problems into a single document that prescribers can use to review medication. Use led to alleviation of patients’ pain, falls, sedation, aggression and confusion, and reduced doses of antipsychotics and sedatives. Our findings indicate that the ADRe Profile works: it empowers nurses and carers through a transfer of useful, necessary, and practical knowledge.
Prescribers’ lack of engagement with service users and reluctance to de-prescribe perpetuates the social distancing, ’othering’, and control of service users. Health problems arising from prescribed medication can be stigmatising and disempowering: antidepressants can cause agitation, nervousness and anxiety, whilst antipsychotics can cause movement disorders and cognitive impairment. Relying on medication to address the problems caused by medication only compounds matters. It can lead to real harm, and places too much power in the hands of those prescribing. As our trials of the ADRe Profile have shown, regulation at the clinical level is insufficient. Healthcare systems need the comprehensive checking of adverse side effects from medicines that the ADRe Profile provides; this leads to improved care and understanding of the impact of ADRs.
Sue Jordan, Meirion Jordan, Patricia Logan, Mojtaba Vaismoradi, David Hughes
Department of Nursing, Swansea University, Wales, United Kingdom
Publication
Adverse Drug Reactions, Power, Harm Reduction, Regulation and the ADRe Profiles
Jordan S, Logan PA, Panes G, Vaismoradi M, Hughes D
Pharmacy (Basel). 2018 Sep 18














Leave a Reply
You must be logged in to post a comment.