Could cancer be cured by inducing an autoimmune disease against It?
Might there be some way to make a microbial protein that the immune system normally overlooks (a “non-antigen”) into a target for an active immune response (an “antigen”)? Could one co-opt the immune system to produce an autoimmune disease specifically against cancer cells? These are possibilities raised by a new paper by Robert Root-Bernstein in Anti-Cancer Agents in Medicinal Chemistry.
One of the ways that pathogens such as malaria avoid the immune system is through “molecular camouflage”: microbes evolve to produce proteins that mimic the proteins of their host. Since the immune system can’t attack the pathogen without attacking its host, it ignores the pathogen. Cancer cells are also too similar to their host’s normal cells to provoke an active immune response. So could one find some way to trick the immune system into “seeing” the pathogen or cancer cells as “different” enough from the host to become targets?
Root-Bernstein likes to read widely, and over a number of years began to realize that people in quite different parts of immunology seemed to have hit upon a common way to activate an immune response against proteins that it normally didn’t “see”.
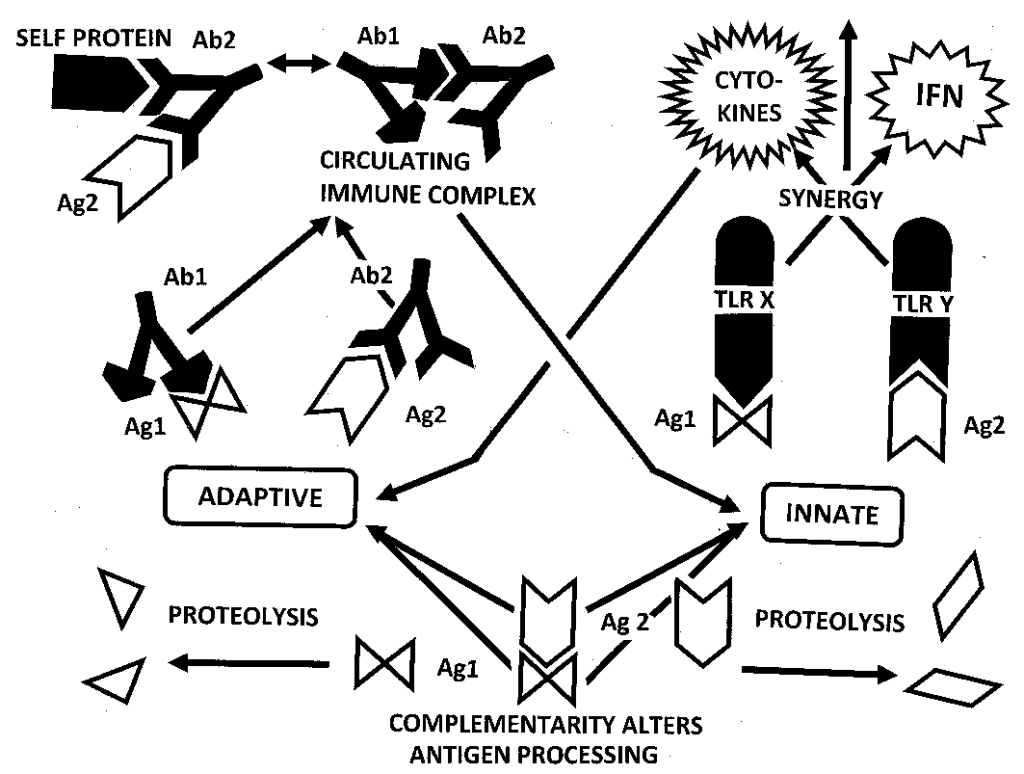
Fig. 1. Proteins that are non-antigenic can be made antigenic by non-covalently complexing them with a molecularly complementary protein. BOTTOM CENTER: Complementary proteins (antigen 1 [Ag1] and antigen 2 [Ag2]) alter antigen processing so that regions of the contributing proteins that would not normally be antigenic become so. In the absence of complementarity, the individual antigens are processed differently (BOTTOM RIGHT and BOTTOM LEFT) so that they are either non-antigenic, or differently antigenic. CENTER LEFT: Complementary proteins induce complementary adaptive immune responses, i.e., idiotype-anti-idiotype antibodies (Ab1 and Ab2)and/or T cell receptors (not shown). Once established, these complementary adaptive immune responses continuously and persistently stimulate each other by mimicking the original antigens. CENTER RIGHT: Complementary proteins also activate complementary toll-like receptors (TLR) and perhaps nucleotide-binding oligomerization domain receptors (NOD) (not shown) that induce a synergistic response resulting in over-production of cytokines and lymphokines (IFN stands for interferons). Thus, each protein acts as an “adjuvant” for the other. The over-production of cytokines and lymphokines (UPPER RIGHT) resulting from synergistic TLR further stimulates antigenicity and/or autoreactivity in otherwise non-antigenic proteins by up-regulating adaptive immunity (arrow from CYTOKINES to ADAPTIVE). Adaptive immunity, in turn (UPPER CENTER), may stimulate further innate activity through circulating immune complexes (CIC) that are formed from complementary antibodies. Complementarity-induced antigenicity will be manifested as an autoimmune response if either or both of the complementary proteins mimic host antigens (UPPER LEFT). Note that the self or host antigen, antigen 2 (ag2), and antibody 1 (Ab1) all mimic each other resulting in confusion within the immune system itself as to what is “self” and “nonself”. In short, complementary proteins alter antigen processing and induce complementary adaptive and innate immune responses that produce a synergistic reactivity that will increase antigenicity and, under some circumstances, break “tolerance”.
What all of these combinations share is that the components are “complementary”. Two molecules are “complementary” when their shapes and charges fit into each other like a hand into a glove or a lock into a key. Antibodies (or antitoxins) are complementary to their antigens. Viruses are complementary to their receptors. Influenza viruses produce proteins that fit like a key into the lock of a protein made by Haemophilus influenzae. Insulin and glucagon are complementary hormones not only in their actions (one lowers and the other raises blood sugar) but also in their structures.
Just how such complementary molecules alter the immune response is not entirely clear. It appears that combinations form complexes that are “seen” by the immune system as something new and dangerous. The complexes certainly are processed differently by the immune system and produce antibodies that the individual components do not. In some cases, it is possible to override the protection systems built into the immune system that normally prevent autoimmune diseases.
So Root-Bernstein proposes two new uses for molecularly complementary complexes. One is to design new types of vaccines against hard-to-vaccinate diseases such as malaria and hepatitis C. The other is to induce autoimmunity directed solely at unique target proteins in cancers so that the immune system can recognize the cancer cells as threats to be eliminated. Both possibilities could usher in a new age of more potent vaccine strategies for controlling and curing diseases that currently evade immunity.
Robert Root-Bernstein
Department of Physiology, Michigan State University, USA
Publication
How to Make a Non-Antigenic Protein (Auto) Antigenic: Molecular Complementarity Alters Antigen Processing and Activates Adaptive-Innate Immunity Synergy.
Root-Bernstein R
Anticancer Agents Med Chem. 2015













Leave a Reply
You must be logged in to post a comment.