Health care utilization for chronic musculoskeletal pain risk: Lessons from the CRASH study
Each year, over four million people go to U.S. Emergency Departments (ED) after a motor vehicle crash (MVC). Although the vast majority of patients are sent home without any serious injuries, many will experience aches and pains such as whiplash and back strains. While many patients get better in the first couple of weeks after an accident, almost half of the people who have gone to the ED after an MVC will continue to have pain several weeks later. The treatment that is started in the ED may impact pain in the weeks to even months after the initial ED visit. Current treatments include physical therapy, pain medications, and behavioral therapy, alone or in combination. After leaving the ED, patients may also receive treatment from their primary care doctor, specialists, or other providers. Currently, it is not known how people use each of these health services as part of recovery from an MVC and what the best course of treatment is.
A study was conducted to understand which health services patients most often use following a MVC. This study included participants from eight hospitals across four states. A total of 793 participants were followed up for one year and were asked to complete a survey on the different types of health services they may have used after their MVC. Participants were divided into high, medium and low risk groups depending on the possibility of them developing long-term pain following their MVC.
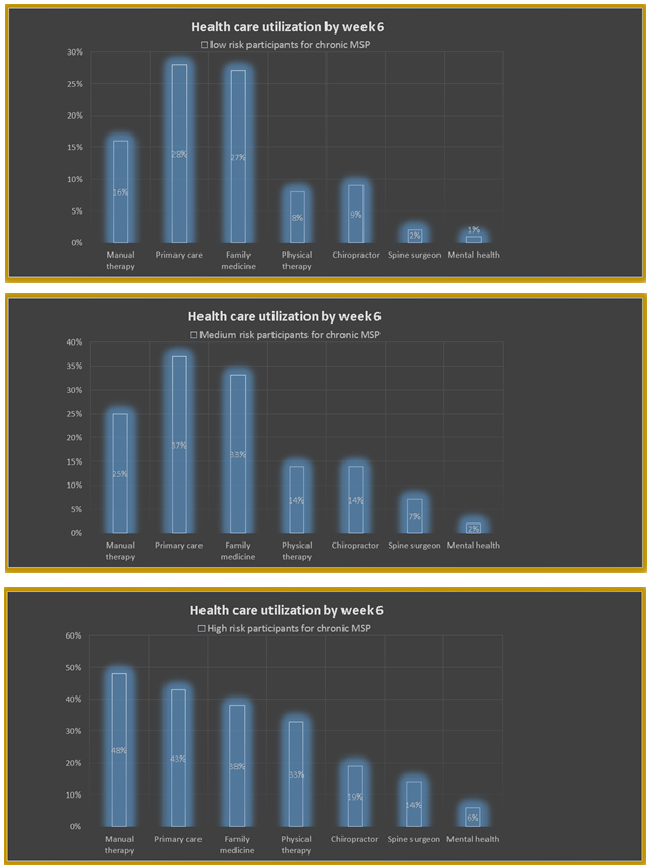
The study findings revealed that participants in the high risk group had a greater chance of developing long-term pain in comparison to those in the medium or low risk groups. It also revealed that across the three groups, some of the most commonly used health services included visits to Primary care, Family medicine, and Physical therapy providers. In comparison, usage of Mental health services was extremely low.
Additionally, the study findings showed that less than half of the participants in the high risk group received appropriate health services. These findings express the need for more organized access to health services for the prevention and treatment of pain in MVC patients. Providing patients with education and referrals to suitable resources may also prevent the over-use of certain health services and avoid unnecessary medication use if pain is controlled in another way. Early access to mental health services may also prevent and improve pain after trauma, but mental health services were rarely used.
There is opportunity in the ED to make timely health services referrals for patients who are discharged home following a MVC, but might be at high risk of negative health outcomes. Future research should be conducted to evaluate if separating people into different risk groups and providing them with differing types of care is both clinically and cost effective. For example, physical rehab, behavioral therapy, and specialty specific services may have better outcomes for patients who have a higher chance of developing long-term pain. In contrast, providing over-the-counter pain-medication and education on the natural course of pain to those with a lower likelihood of developing long-term pain may avoid unnecessary care.
Taha Feroze, Tarek Nizami, Evelyn K Nimaja, Francesca L. Beaudoin
Department of Emergency Medicine, Alpert Medical School of Brown University, Providence, RI, USA
Publication
Health care utilization following motor vehicle collision is poorly stratified by chronic pain risk: Lessons from the CRASH study.
Beaudoin FL, Rosellini AJ, Bortsov A, McLean SA
Am J Emerg Med. 2019 Mar













Leave a Reply
You must be logged in to post a comment.