Nutritional strategies in managing postmeal glucose for Type 2 Diabetes mellitus
The postmeal hyperglycemia is a common feature of Type 2 Diabetes (T2D) with the majority of the patients have not achieved the postmeal target of less than 7.8 mmol/L at 2h. While the role of Medical Nutrition Therapy to improve the overall glycemic level has been established, the specific strategies to achieve optimal postmeal glycemic level is uncertain. In this review, we aim to identify specific nutritional approaches that optimise the postmeal glycemia for patients with T2D. Identification of optimal approaches may guide healthcare professional in their recommendation to lead T2D patients in achieving optimal postmeal glucose.
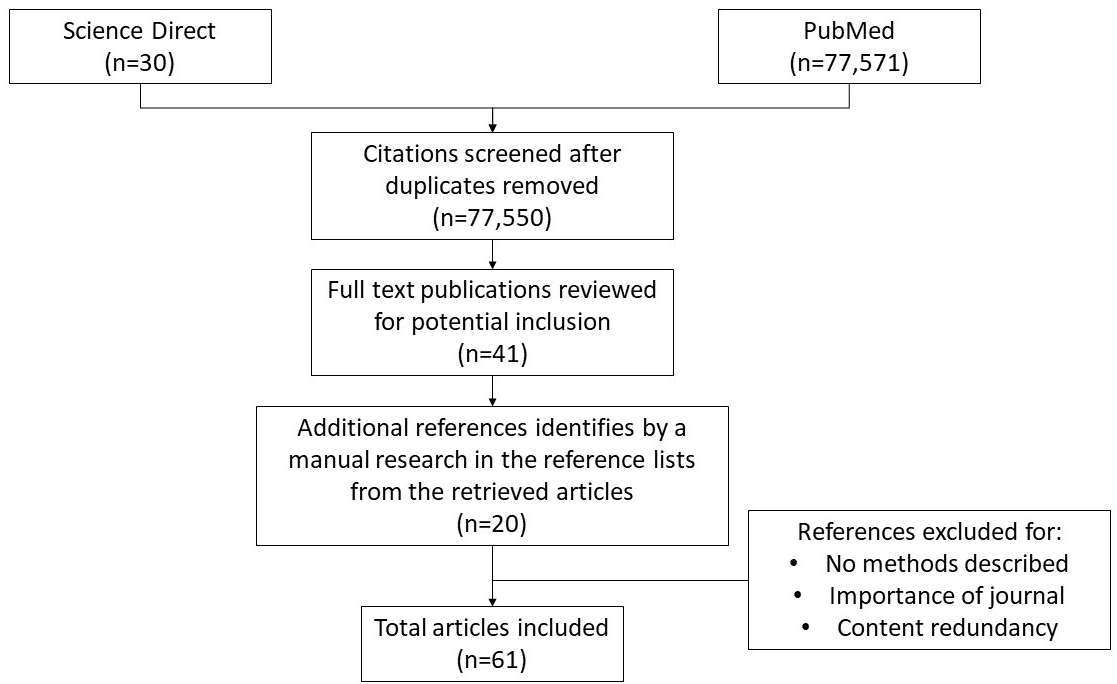
The literature search was conducted using multiple databases for studies examining the nutritional strategies to manage postmeal glycemia in patients with T2D. We utilised the Medical Subject Headings terms and restricted to study related only to humans, published in English from year 2009 to 2019.
This review indicates that postmeal hyperglycemia can be modulated with four nutritional approaches.
Utilizing the appropriate amount and selecting right type of carbohydrate
Dietary carbohydrate is the main macronutrient influencing the postmeal glycemic level especially in patients with T2D. Dietitian will advice patients with T2D to control on the portion size of carbohydrate to manage their blood glucose level. In order to optimize the glycemic control, the type of carbohydrate which is assessed by the Glycemic Index (GI) and Glycemic Load (GL) can be implemented.
GI provides ranking to a specific food based on the postmeal blood glucose response; whereas GL combines both amount and GI of carbohydrate foods. Numerous studies had demonstrated the effectiveness of low GI diet in improving postmeal glycemic response among T2D patients.
The mechanism underlying this diet can be explained by the slower rate of gastric emptying, lead to slower rate of carbohydrate absorption in the GIT, thereby compensating the delay in insulin secretion and insulin resistance.
Specific dietary protein
The magnitude of the postprandial glycemic spike is affected by the dietary protein. This is known as the mixed meal effect, where protein slowed the gastric emptying process, thereby delayed the peak glucose response and sustained the release of insulin by pancreatic β-cell. Whey protein is a fast-acting protein and exerted insulinotropic effect. The bioactive peptides in whey stimulated the incretin effect and increased GLP-1 production in the gastrointestinal tract, thus induced insulin secretion by the pancreatic β-cell.
Manipulating meal timing and orders
Interestingly, recent research has paid particular attention to the circadian rhythm and meal timing. Breakfast consumption can affect the glycemic fluctuation not only at the postmeal state but the subsequent meal of the day. This can be explained by “second meal phenomenon”. Moreover, manipulating the temporal meal sequence can delay gastric emptying rate and enhance insulin secretion through incretin effect.
Others (promoting postmeal physical activity, incorporating diabetes-specific formula and certain functional foods)
A postmeal walk is an effective strategy to mitigate postmeal glycemic excursions. Exercise is clinically evidenced to improve insulin sensitivity, increase glucose uptake in skeletal muscle and decrease hepatic glucose production.
There has been an increasing interest in determining the effect of diabetes-specific formula (DSF) in the postmeal glucose management in patients with T2D. The DSF is specially formulated to suit the nutritional requirement of T2D patients. There are several properties of the DSF: low GI, high fiber, blend of high-quality protein (50% whey and 50% casein) and special fat blend of monounsaturated fatty acids (MUFA) and polyunsaturated fatty acids (PUFA).
The functional food such as berries and nopal is usually identified as traditional medicine where their positive impact observed was likely to be related to the bioactive compound that inhibit the activity of carbohydrate digestive enzyme, lead to slower absorption of glucose in the GIT and modulate postmeal glucose metabolism.
In conclusion, postmeal hyperglycemia warrants to be highlighted in the management of patients with T2D. Before proceeding to pharmacologic treatment, improvement in several nutritional aspects shown to exert immediate favourable changes in postmeal hyperglycemia. The array of nutritional approaches provides a suite of intervention options for the management of postmeal hyperglycemia in patients with T2D by the healthcare professional.
Lau Zhi Ch’ng
Department of Nutrition and Dietetics, Faculty of Medicine and Health Sciences, Universiti Putra, Malaysia
Publication
Nutritional strategies in managing postmeal glucose for type 2 diabetes: A narrative review
Lau Zhi Ch’ng, Mohd Yusof Barakatun-Nisak, Wan Zul Haikal Wan Zukiman, Faridah Abas, Norasyikin A Wahab
Diabetes Metab Syndr. Jul-Aug 2019













Leave a Reply
You must be logged in to post a comment.