Plasma cell myeloma: an integrated diagnosis of multiple dimensions
Plasma cell myeloma, a neoplastic proliferation of plasma cells, is one of the most common malignancies in the world. The clinical symptom and treatment response of individual patient are variable, which may relate to the underlying heterogeneous pathology and biology of each tumor. Myeloma cells show mature or immature morphology, and somatic TP53 aberrations are associated with immature plasma cell morphology. Previous studies have demonstrated an important prognostic value of chromosomal alterations. Myeloma Prognostic Risk Signature (MyPRS) based on gene expression profiling and molecular subtype analysis, may stratify patients into high-, high risk-borderline, low-risk borderline, and low-risk categories to optimize individual treatment. The goal of our study is to integrate the histology, MyPRS score, and gene mutation analysis by next generation sequencing, for a diagnosis of plasma cell myeloma.
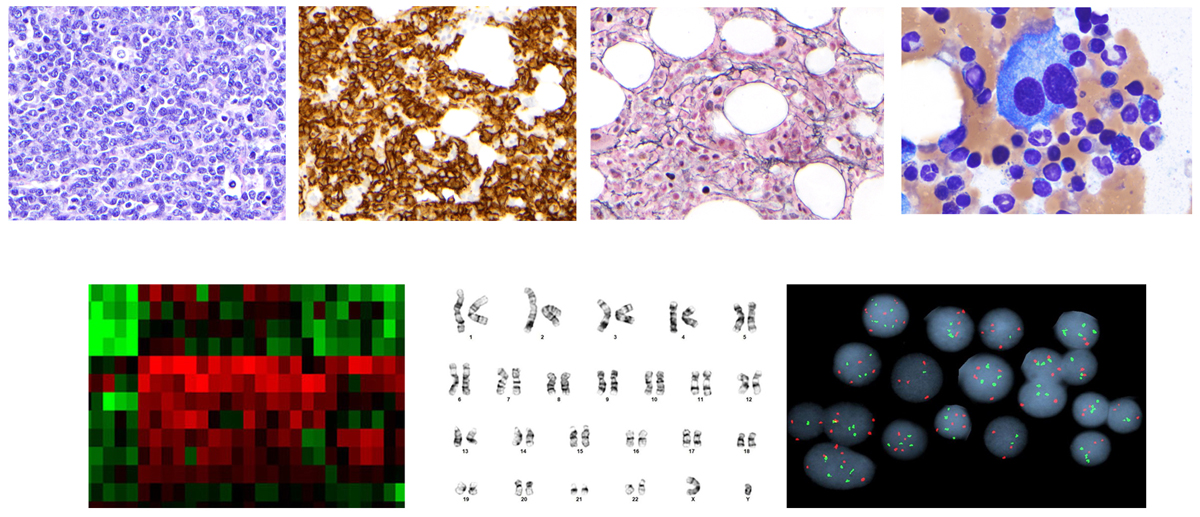
We firstly stratified our patients into high risk and low risk groups based on MyPRS scores. Next, we demonstrated that cases with MyPRS high risk score exhibited specific histologic features including higher bone marrow cellularity, higher tumor burden, sheet like growth pattern, immature morphology, higher mitoses, and increased fibrosis, that correlate with poor clinical outcomes. Furthermore, in this study, we reported the recurrent mutations of the Ras/ MAP kinase pathway equally distributed in both high risk and low risk cases, suggestive of important role of this pathway in the tumorigenesis in myeloma patients but nor tightly associated with patient’s prognosis. Interestingly, the mutations involving the epigenetic modifiers, DNMT3A and TET2, were also identified in patients of both groups.
In addition, two mutated genes, TP53 and CD36, were closely associated with the high risk cases in our study. 17p loss identified by FISH study did not show significant difference between high risk and low risk cases. However, cases with concurrent TP53 mutation and 17p loss appear to have more diffuse growth pattern, immature cell morphology, and higher mitotic index, which may relate to the potential bi-allelic dysfunction of TP53. Consistent with our findings, recent studies have shown that myeloma patients with bi-allelic inactivation of TP53 is associated with much poor prognosis than the ones with wild-type or mono-allelic inactivation.
In summary, we studied the morphological, chromosomal alterations, and somatic mutations in a large group of myeloma patients, and their difference between MyPRS high risk and low risk cohorts. Our study provides an example and insights of an integrated diagnosis system for clinical practice.
Jinjun Cheng, Julie Teruya-Feldstein
Hematopathology Services
Icahn School of Medicine at Mount Sinai
One Gustave L. Levy Place, Box 1194 New York, NY 10029, USA
Publication
Bone marrow morphologic features, MyPRS, and gene mutation correlations in plasma cell myeloma
Yansheng Hao, Daniel Khaykin, Levi Machado, Tayler van den Akker, Jane Houldsworth, Bart Barlogie, Shafinaz Hussein, Siraj M El Jamal, Bruce Petersen, Julie Teruya-Feldstein
Mod Pathol. 2020 Feb













Leave a Reply
You must be logged in to post a comment.