Three-step method for the frozen elephant trunk positioning by transesophageal echocardiography
The frozen elephant trunk (FET) procedure has prevailed because it has simplified the treatment of complex thoracic aortic lesions. However, some procedure-related complications have been reported, and spinal cord injury is one of the most important complications. The exact mechanism of spinal cord injury in FET interventions is not fully understood. Stent graft length, thromboembolism, and spinal cord ischemia time during total circulatory arrest are considered as determinants of clinical outcomes. In our hospital, 80 patients with the FET procedure (acute aortic dissection 34, chronic aortic aneurysm 14, and true thoracic aneurysm 32) had no spinal cord injury. Although it is unknown whether the mechanism of spinal cord injury is the same in both aortic aneurysm and dissection, the FET was implanted according to the same technique and concept as conventional method. There are three key points to avoid spinal cord injury: (1) the distal end of stent graft should be positioned up to the eighth thoracic vertebrae level; (2) the time for selective left subclavian artery (LSA) perfusion and distal body circulatory arrest should be shortened within 60 min; and (3) mean systemic blood pressure should be maintained above 70 mmHg. Especially, Key point (1) is the most important. The Adamkiewicz artery that supplies blood to the spinal cord originates from the descending aorta below the eighth thoracic vertebrae level in general.

Fig. 1. Step2: Marking the TEE probe at aortic valve level
After the aortic valve was visualized at the center in mid esophageal aortic valve short axis view of TEE, the probe is rotated a half turn (descending aorta short axis view of TEE) and descending aorta at aortic valve level is visualized at the center. The TEE probe in the corner of mouth is marked at this position because we can’t confirm the descending aorta at aortic valve level during circulatory arrest.
ME AV SAX: mid esophageal aortic valve short axis view
D-AO SAX: descending aorta short axis view
Therefore, it was assumed that the distal end of the stent graft should be positioned at an upper level than the eighth thoracic vertebrae. For the cases of aortic dissection, one of the stent grafts with a length of 6 or 9 cm was selected, after measuring the length by setting a bench- mark around the seventh thoracic vertebrae level to enable the stent graft implantation in the straight part of the aorta, with the aim of reducing the stress on the intima as much as possible. The level of aortic valve, which usually locates around the seventh thoracic vertebrae level, was an appropriate benchmark. Three-step method for transesophageal echocardiography (TEE)-guided implantation of FET is shown below.
Step 1 Determination of stent graft size and position.
The size and position of the stent graft were determined by preoperative CT scan. At the same time, the distance between the aortic valve and the scheduled distal end position of stent graft was accurately measured.
Step 2 Marking the TEE probe at aortic valve level (Fig. 1).
After the aortic valve was visualized at the center in mid-esophageal aortic valve short-axis view of TEE, the probe was rotated a half turn (descending aorta short-axis view of TEE) and descending aorta at aortic valve level was visualized at the center. The TEE probe in the corner of mouth was marked at this position because the descending aorta at aortic valve level was not confirmed during circulatory arrest.
Step 3 TEE guided-implantation of FET (Fig. 2).
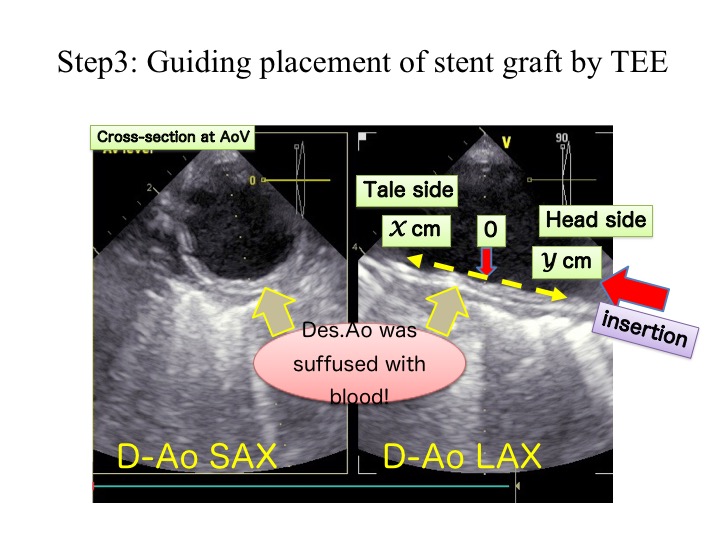
Fig. 2. Step3: Guiding placement of stent graft by TEE
TEE is located at the aortic valve level (marking in mouth corner) and JGOS is visualized at the center. At first, we depict the short axis view as circle. Next, we depict the long-axis view as horizontal. As the descending aorta is often kinking or awkward, the ideal depiction on both views is difficult. In this case, we have priority of the short axis view. the long-axis view was depicted slightly obliquely in the case. The difference of depths of the TEE probe between these 2 levels is defined as the distance from the aortic valve. JGOS is deployed at scheduled distance from the aortic valve level under guidance of TEE.
ME AV SAX: mid esophageal aortic valve short axis view
D-AO SAX: descending aorta short axis view.
The J Graft open stent (JGOS) graft (Japan Lifeline, Tokyo, Japan) [5] introduced into the aorta was depicted as a strongly echogenic line accompanied by an acoustic shadow with the stent-graft packed inside. When JGOS was directed to the aortic wall or the intimal flap, JGOS was reshaped and inserted again. At first, TEE was located at the aortic valve level (marking in mouth corner) and JGOS was visualized at the center. The difference of depths of the TEE probe between these two levels was defined as the distance from the aortic valve. JGOS was deployed at a scheduled distance from the aortic valve level under the guidance of TEE. Usually, Foley balloon catheter was not inflated to avoid an intimal injury. Although the diameter of JGOS was initially shorter, JGOS gradually inflated with recovery of distal perfusion.
Kazuo Yamanaka
Executive Director, Cardiovascular Center, Nara Prefecture General Medical Center, Nara, Japan
Publication
Three-step method for transesophageal echocardiography-guided implantation of the frozen elephant trunk: how to prevent spinal cord injury.
Yamanaka K, Ishii H
Gen Thorac Cardiovasc Surg. 2019 Mar













Leave a Reply
You must be logged in to post a comment.