Heart medication and metabolism: What physicians should reflect on to keep them in harmony
Cardiovascular diseases are the leading cause of death globally and have been for a long time. This spotlight has ensured that doctors treating patients with heart problems have a wide variety of medications to work with. Most of the time, these medications are used to address direct and immediate problems the heart is dealing with. The catch is that apart from this direct and intended effect, heart medications have additional and easier to overlook effects on the metabolism. A recent review article (1) has described how commonly prescribed heart medications could be making both beneficial and harmful changes in the metabolism of the heart and the rest of the body. These changes are important for physicians to be aware of to make sure that they are doing the most good and the least harm when deciding what medications to prescribe.
Metabolic derangements have long been recognized as playing an important role in the pathophysiology of cardiovascular diseases. Metabolic impairment is not just a feature of the heart, but rather a global issue with important contributions from organs and peripheral tissues. Prescription of cardiac medications is aimed towards the pathophysiological mechanisms underlying the disease process. For instance, inhibition of the renin–angiotensin–aldosterone and sympathetic nervous systems is directed towards ameliorating abnormal neuro-hormonal activation. However, apart from their primary therapeutic actions, these drugs may positively also affect the global and cardiac metabolism. Similarly, a positive ancillary metabolic effect has also been observed with ARNI (angiotensin receptor neprilysin inhibitor), acetylsalicylic acid, trimetazidine, ranolazine, ivabradine, alpha blockers, central sympathetic inhibitors. On the contrary, among the others, thiazide diuretics, mineral corticoid receptor antagonists, calcium channel blockers, unfractionated heparin, direct thrombin inhibitors, specific statins, have all been shown to impair different metabolic functions. In this context it is interesting to note the recent demonstration of the beneficial effect of sodium-glucose transport protein 2 inhibitors (SGLT2i) in diabetic and non-diabetic in cardiac patients, indicating that the cardiovascular effects of these drugs are largely independent from glucose lowering. These findings will necessarily lead to the need to re-consider this class of drugs not as solely a glucose lowering drug but as metabolic cardiovascular drugs.
Overall, it is clear that additional pharmacological actions may be of special interest for both potential beneficial and deleterious effects and should be well understood and known by all providers managing patients with cardiovascular diseases. In table 1 are a few examples of effects from commonly prescribed medications in cardiac patients.
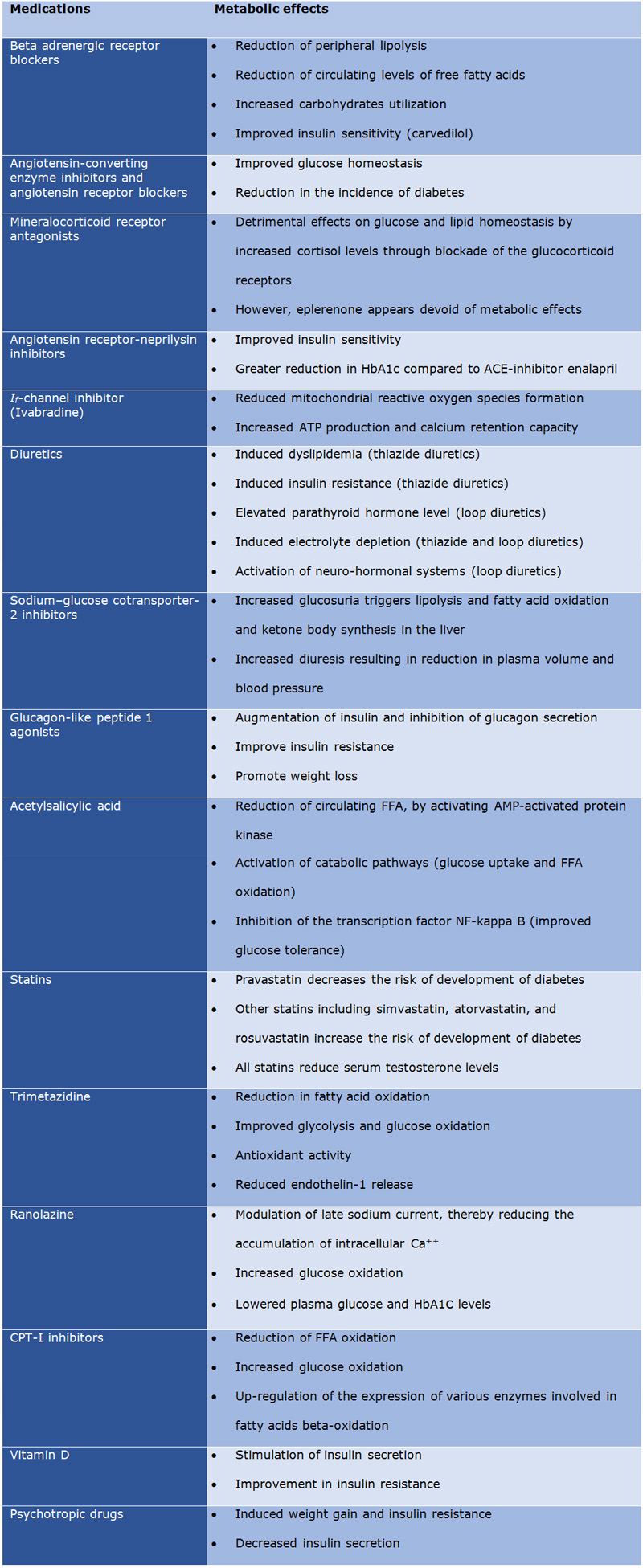
Tab. 1. Main metabolic effects of medications used for the treatment of patients with heart failure.
Legend: ACE: angiotensin-converting enzyme; AMP: adenosine monophosphate; ATP: adenosine triphosphate; CPT-I: Carnitine palmitoyl transferase I; FFA: free fatty acids; HbA1c: glycated hemoglobin, NF-kappa B: nuclear factor-kappa B.
In conclusion, most routinely used cardiovascular drugs yield ancillary energy metabolic effects that can either be beneficial or detrimental. Metabolic effects may be peripheral and/or directly influencing cardiac metabolism. Physicians looking after cardiovascular patients should be aware of the ancillary effects of the main drugs used in the daily clinical practice. Some of these metabolic properties may represent a principal effect of single drugs. All these concepts should prompt us to monitor peripheral and cardiac metabolic levels and try to improve them. Evidence-based medicine takes into account the beneficial effects of drugs on hard end-points, obtained by clinical trials of relatively short duration and it cannot be excluded that over longer time periods these beneficial effects of drugs could be either eliminated or reinforced due to their ancillary energy metabolic effects. For these reasons, future trials of cardiovascular drugs should take into account the evaluation of specific action on metabolism in order to better define their prescription in cardiac patients with different metabolic risk profiles.
Alexandru V Florea 1, Roberto Spoladore 2, Gabriele Fragasso 1,2
1Università Vita-Salute San Raffaele, Milan, Italy
2Clinical Cardiology – Heart Failure Clinic, Ospedale San Raffaele, Milan, Italy
Publication
Metabolic effects of cardiovascular drugs.
Fragasso G, Margonato A, Spoladore R, Lopaschuk GD
Trends Cardiovasc Med. 2019 Apr
Related Articles:
 | Systemic therapy in juvenile localized scleroderma Juvenile localized scleroderma, also known as morphea, is an rare condition, it occurs around 1 in 5000 children, where the skin and the tissues underneath the skin like fat tissue,… |
 | Could mometasone furoate be a viable glucocorticoid… Glucocorticoids are medications widely used to treat inflammation and allergies, and in contexts of immunosuppression such as after transplants. They are well-established and safe. The problem is that, when used… |
 | Looking inside the heart: how multiple chronic… The aim of this study was to understand how having several ongoing health problems—what we refer to as multimorbidity—impacts the heart in people with cardiovascular disease, especially those undergoing heart… |
 | Unlocking new treatments for bone diseases: using… Despite appearances, bones are a constantly changing organ in the body. Cells that produce new bone (named osteoblasts) and cells that break down bone (named osteoclasts) work in harmony to… |
 | Ferrate technology: an innovative solution for… Sewers might be out of sight, but they play a huge role in shaping the well-being of a society. They quietly carry away all the wastewater from our homes, businesses,… |
 | Making Christmas trees under duress, or how cells… Some of the most enduring images for a molecular biologist are electron microscopy micrographs of the so-called “Christmas trees”, famously first observed by Oscar Miller from newt oocytes in 1969.… |







Leave a Reply
You must be logged in to post a comment.