Clubbing in patients with fibrotic interstitial lung diseases
Many years ago Hippocrates already described clubbing. Clubbing is a deformation of the nail base resulting in a swollen and spongy convex. It is frequently seen in patients with interstitial lung diseases (ILDs). ILDs contain a variety of diseases affecting the alveoli (diffuse end of the respiratory tree were gas exchange with the blood vessels takes place) and the pulmonary interstitium. The interstitium is the space between the alveoli and blood vessels. A significant proportion of these diseases are characterized by progressive pulmonary fibrosis, of which the most common form is idiopathic pulmonary fibrosis (IPF). IPF is a deadly disease with a median survival of 3–5 years without treatment. Patients with pulmonary fibrosis experience symptoms of breathlessness, cough and fatigue. Physical examination often reveals fine bibasilar inspiratory crackles and finger clubbing.
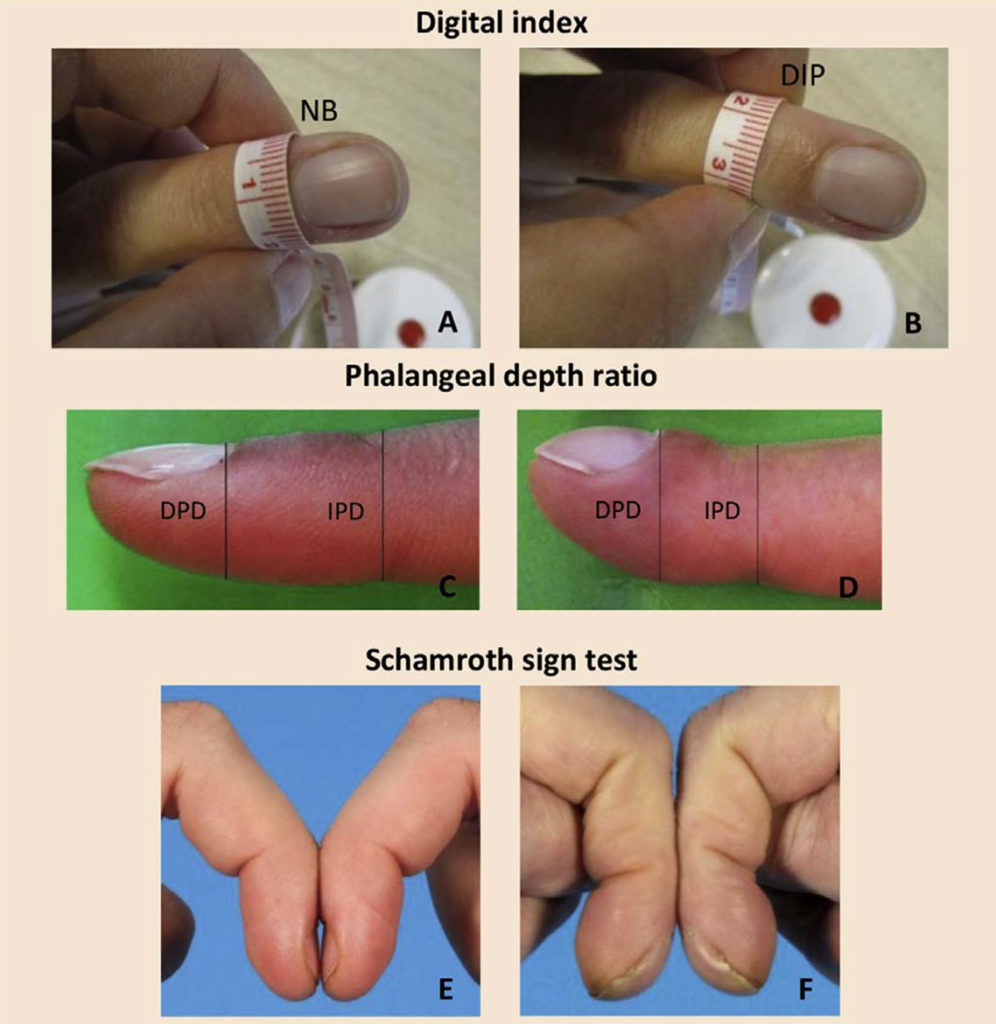
A. Measuring circumference of NB
B. Measuring circumference of DIP
C. Normal finger with DPDIPD
E. Diamond-shaped window: negative
F. No diamond-shaped window: positive NB, nail bed;
DIP, distal interphalangeal joint; DPD, distal phalangeal depth; IPD, interphalangeal depth. Digital index = NB:DIP ratios for all 10 fingers. Phalangeal depth ratio = DPD:IPD ratio.
In IPF, clubbing is associated with poor prognosis, but little is known about the best methodology to assess clubbing in ILDs. Hence, the prevalence, clinical utility and clinical significance of clubbing is unknown. We therefore aimed to evaluate the agreement between different clubbing assessment methods in patients with fibrotic ILDs. Additionally, we assessed the prevalence of clubbing in different fibrotic ILDs and related clubbing to disease severity and quality of life.
Consecutive outpatients with fibrotic ILDs of two tertiary referral centers were included. Clubbing was assessed with the phalangeal depth ratio, the digital index, the Schamroth sign test, and at sight by the treating physicians and investigator (Fig. 1). Additionally, patients completed patient-reported outcomes (PROMs) on quality of life and symptoms.
We included 153 patients with fibrotic ILDs (68 IPF patients) of two tertiary referral centers, with a mean age of 65 (range 33–88). Pulmonary function was measured in all patients. The mean forced vital capacity (FVC) was 79% (25–145%), and mean transfer capacity for carbon monoxide corrected for hemoglobin (TLCOc) was 50% (16–104%).
We found no to weak agreement on the presence of clubbing between the different clubbing measuring methods. Strikingly, the assessment of clubbing by the physician and investigator showed a much better agreement. Clubbing prevalence varied according to the method used, ranging from 7-42% in the total group of patients and 7-52% in IPF. The degree of clubbing did not correlate with disease severity, measured by lung function parameters FVC or TLCOc (p > 0.2) or with quality of life scores. Although clubbing is considered an important clinical feature in ILDs, assessment methods for clubbing showed no to poor agreement. Clubbing was present in 7–42% of our fibrotic ILD cohort and showed no correlation with disease severity and quality of score. Further studies are therefore needed to gain more insight into measuring clubbing reliably and the possible prognostic value and evolution of clubbing.
Mirjam van Manen, Catharina Moor, Marlies Wijsenbeek
Department of Respiratory Medicine, Erasmus University Medical Center, Rotterdam, The Netherlands
Publication
Clubbing in patients with fibrotic interstitial lung diseasesVan Manen MJ, Vermeer LC, Moor CC, Vrijenhoeff R, Grutters JC, Veltkamp M, Wijsenbeek MS
Respir Med. 2017 Nov













Leave a Reply
You must be logged in to post a comment.