Fatty liver disease: a condition caused by modern day lifestyle
Non-alcoholic fatty liver disease (NAFLD) refers to the build-up of fat (steatosis) in the liver that occurs in the setting of obesity and/or diabetes. Specifically, other causes such as alcohol excess or drugs or genetic conditions need to be excluded to make the diagnosis. As global levels of obesity increase, so the incidence of NAFLD increases. The range of severity of NAFLD is illustrated in Figure 1, with non-alcoholic steatohepatitis (NASH) representing a more severe form of fatty liver disease. NASH includes not just fat but also the presence of inflammation and fibrosis which can ultimately lead to progression to liver cirrhosis and cancer.
The factors resulting in patients developing progressive damage in the setting of NAFLD are not fully understood – the presence of multiple hits causing liver injury seems to be the key. The main driving force of the injury is insulin resistance (IR) which results in an increased breakdown of lipids/triglycerides in the adipose tissue and their subsequent release into the blood circulation and then the liver.
These toxic fats [glycerol and free fatty acids (FFA)] build up in the liver and are viewed as the first hit of liver injury which then triggers a further cycle of cellular injury and death. As a result, the liver injury progress from just build-up of fat to the development of NASH. Recent genetics studies have identified possible genes [PNPLA3] that may identify patients that are more likely to progress to develop more advanced liver damage.
A key in the assessment of a patient with NAFLD is to establish the absence or presence of fibrosis or liver scarring. This is important as patients with only fat and no evidence of inflammation or liver scarring do not seem to be at increased risk of developing significant liver disease. The presence and level of liver scarring can be monitored using blood tests or liver scans with liver biopsy reserved for more definitive assessment.
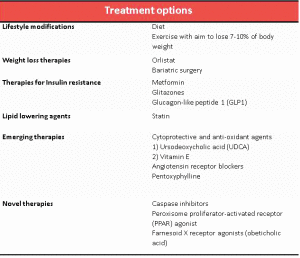
There are no licensed therapies specifically for the management of NAFLD, and therefore current approaches are based on lifestyle management and management of associated co-morbidities in anticipation of future pharmacological developments. There are many ongoing trials in the field of NAFLD as summarised in Figure 2 and it is anticipated that new therapies will be available for use in clinical practice in the next 3-5 years.
Publication
Non-alcoholic fatty liver disease: when to intervene and with what.
Than NN, Newsome PN
Clin Med (Lond). 2015 Apr














Leave a Reply
You must be logged in to post a comment.